What is a wart? We will analyze the causes of occurrence, diagnosis and methods of treatment in an article by a dermatologist with 37 years of experience.
Definition of disease. Causes of the disease
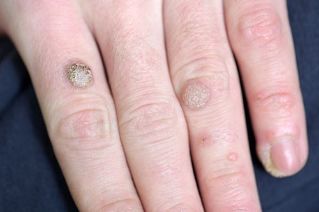
Wartsare benign benign skin lesions in the form of local overgrowth of the upper layer of the skin (epidermis) with papules (nodes) or plaques.
The incidence of warts in adults is 7-12%, in children of school age - up to 10-20%.Warts are very similar to other skin growths. It is not usually possible for a person to determine the disease accurately on their own, so a dermatologist must be consulted to make a diagnosis.
Warts are caused by the human papillomavirus. The type of virus affects the type of warts that can develop. Thus, all types of human papillomavirus virus infect tissue at its most characteristic localization.
| HPV type | Option localization |
Types of warts |
|---|---|---|
| 1 | Feet, Knees, Palms, hands, fingers |
plantar and palmar warts, simple warts |
| 2, 4 | Hands, fingers, knees, as often - feet |
simple warts, occasional plantar, palmar and mosaic warts |
| 3, 10 | Shins, hands, face | flat warts |
| 7 | Hands, fingers | Butcher Warts |
| 5, 8, 9, 12, 14, 15, 17, 19-24 |
Face, arms, front torso |
Epidermodysplasia verruciform |
Virus infection usually occurs through contact - with direct contact between infected and healthy skin (for example, while shaking hands) or indirectly (through handrails, toys, etc. ). Therefore, you can become infected with the human papillomavirus virus, which causes warts, in a wide range of places - in public transport, at school, at work, at home, in places with high contact andhumid environment (swimming pools, saunas, gyms). Minor trauma to the epidermis, through which viruses enter, as well as inflammation of the skin, contributes to the infection.
Adding to the appearance of warts too:
- immunodeficiencies
- (including HIV infection); Warm and humid environment
- ;
- the need for professional contact with meat and fish ("butcher warts").
Some types of human papillomavirus are transmitted from parents.
But despite the horror stories that we are so afraid of in our youth, they cannot be infected - this is one of the most common myths about this disease, which has no basis.
If you find similar symptoms, consult your doctor. Do not self-medicate - it is dangerous for your health!
Wart signals
The signals will vary depending on the type of wart.
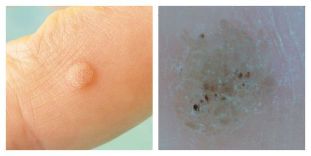
common wart:
- Round compact papule of normal color, 1-10 mm and larger.
- The surface of the papule is covered with cracks, layers.
- If the papule is on the finger, then the font disappears and is distorted. Same for the palm drawing.
- Simple warts are located alone or in several pieces - they are usually seen in the areas of greatest injury (hands, fingers, knees).
- When viewed with a dermatoscope, the doctor may see small brown dots - thrombosed (clogged) capillaries. Patients often refer to these points as “roots”. This is the main sign for a doctor: a dermatologist can use it to distinguish a wart from other similar diseases (for example, molluscum contagiosum and keratoma).
Plantar wart (horned):
- The main symptom that usually causes a patient to see a doctor is pain while pushing and walking.
- Such warts are usually localized on the feet.
- When a doctor is contacted, as a rule, a keratinized, uneven plaque of the usual color appears, although at the first stage you see a fairly smooth papule. With keratinization, the capillaries can only be seen if the keratinized layer of the skin is removed. The skin of the fair is distorted.
- Plantar warts are usually solitary, but there are also 2-6 warts;
- These warts are often confused with corn (especially dry) - this is the description of the problem that patients usually have.
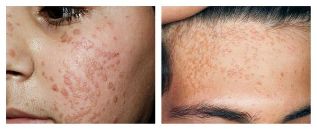
Flat wart (young):
- It appears to be a round, clear, smooth papule of normal color, pink or brown, 1-5 mm in size.
- It appears on hands, on shins, often on the face.
- There are always some such warts - they are located in groups.
Verruciform epidermodysplasia (senile wart):
- Large, round, numerous neoplasms of normal color, pink or brown.
- They are often seen on the face, arms, in front of the torso.
- May be mixed with keratoma, shale and skin cancer.
Pathogenesis wart
Once it enters the body, the human papillomavirus can remain in a latent state for a long time - usually one does not even know it exists. When favorable factors for the virus appear, it begins to “multiply” in the epitheliiam, resulting in tissue changes.
Unlike other viruses, the human papillomavirus does not destroy the cells of the epitheliiam themselves - they die alone, naturally, in the process of keratinization and flaking.
Local factors and the state of the immune system influence the spread of the infection. For example, people with HIV infection or a kidney transplant are more likely to develop warts. Moreover, these neoplasms are often difficult to treat. With normal immunity, the virus does not affect the deep layers of the skin, so many people get warts on their own after a few months.
The main step in the appearance of warts is the acceleration of the rate of cell division and growth with the help of the virus. This rapid metabolism leads to thickening of the skin layers. Since the tissues grow in a small, certain area, a tube appears, called a wart.
Classification and stages of development of the wart
The classification of warts is not generally accepted. However, there are some common types:
- The common wartis the most common type (only 70% of warts are). Such neoplasms do not feel and only cause aesthetic discomfort.
- Plantar wart- seen on the soles of the feet, it is painful, therefore it needs treatment. Skin trauma due to uncomfortable, tight, chafing shoes contributes to the development of such a wart.
- Flat warts- seen more often in young people, teenagers. This is due to the unstable hormonal background of young people, which affects the whole body. Flat warts are usually almost invisible.
- Senile warts- typical for the elderly. They are often seen on the part of the body covered with clothes, but they can occur on the face and hands. If there is no discomfort, such warts should not be treated - medicine in the elderly can be much slower than in young people, due to a slow metabolism.
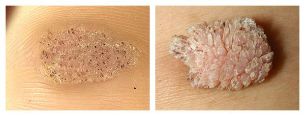
Other authors distinguish more from these types of warts:
- mosaic warts(HPV 2, 4) - neoplasms on the palms and soles. They look like foci of hyperkeratosis, i. e. thickening of the stratum corneum (usually in the front leg), covered with deep cracks.
- Cystic warts are a very rare type of foot neoplasm (HPV 60). It is a soft knot with cracks. Open, a white-yellow discharge is visible, resembling curd.
- warts "butchers"(HPV 7) - seen on the hands and fingers of people who are constantly in contact with meat and fish. Presented as hypertrophied neoplasms similar to cauliflower, but of normal color.
In addition, types of warts are distinguished depending on their location.
Thus, anogenital warts are a common disease - tumor-like neoplasms that appear on the genitals (especially in places where the skin moves to the mucous membrane). Types 6 and 11 are usually caused by HPV.
Complications of the wart
The main reason patients with warts go to the doctor is an aesthetic defect that can affect the patient’s quality of life, self-confidence and the development of many complexities. Complications can include cracking of the wart surface and adding infection, and in some types of warts, saline while walking.
Skin warts do not usually dissolve into malignant neoplasms, they are quite harmless, however, in very rare cases, such a complication can occur in people with suppressed immune systems.
Other difficulties arise when trying to remove neoplasms on their own. In this regard, inflammation and aesthetic defects may occur in the form of scars, as well as further spread of the virus through the skin, because, in the morning after removing one wart by itself, one may wake up with severalnew.
Remember that, under the shadow of a wart, it is possible to hide a completely different disease, which can not be determined without the advice of an experienced doctor.
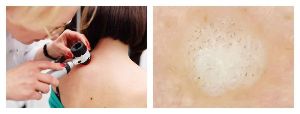
Wart Diagnosis
Examination (clinical picture) and anamnesis (medical history) are usually sufficient to make a diagnosis.
To confirm the diagnosis, the doctor may perform a histological examination - a study of the cells of the neoplasm.
It is very important to make a differential diagnosis - to distinguish between warts and other diseases. For example, common warts need to be distinguished from the following diseases:
- Molluscum contagiosum- appears more frequently on the body and genitals, less often on the hands and feet. Hemisphere is implied by the surface; when pressed from the sides, a white “gruel” is released.
- Epidermal verrucous nevus- often solitary, a person is from birth. It rises above the surface of the skin, often covered with hair.
- Basalioma- a tumor in the form of a cylinder of nodes, covered with a crust in the center. It is common for the elderly.
Palmar-plantar wartsmust be distinguished from the following diseases:
- Keratoderma- major areas of keratinization and inflammation of the skin. No coagulation capillaries.
- Palmar-plantar syphilis- multiple painless neoplasms, exfoliates skin along the periphery. Syphilis has a positive reaction
- Cup- usually painless, it can only cause pain by pushing it vertically.
The doctor must distinguish other types of warts from some diseases. If other pathology is suspected, it may prescribe additional diagnostics (for example, detection of antibodies to viruses, CT or MRI).
Wart treatment
Warts are treated for aesthetic purposes and to improve the patient's quality of life. It can only be prescribed by a doctor after an accurate examination and diagnosis. Independent efforts to get rid of a wart are not accepted, as a patient without medical education and the necessary equipment is not able to accurately determine the disease, and complications after such “treatment” are much more frequent than recovery.
There are several ways to treat warts. All are usually performed under the supervision of a doctor, and some - only in the clinic's treatment room.
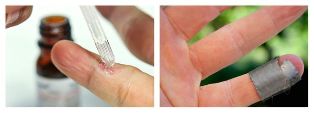
Chemical Healing
Milk-salicylic collodion and salicylic patches are used to get rid of the wart. The percentage of drugs and method of use (long-term use of patches, application, etc. ) depends on the prevalence and localization of the neoplasm.Zinc and 2-chloropropionic acid solutions can also be used. In this case, a chemical composition is applied to the pre-treated surface, which is left on the wart until the color changes (depending on the type of wart). The procedure is repeated after 7, 14 and 21 days. Before each procedure, the tissue is removed mechanically.
Another chemical method is a mixture of nitric, acetic, oxalic, lactic and copper nitrate nitrates. In this way, only relatively small neoplasms - up to 5 mm - are treated. The solution is also left to change the color of the wart. After 3-5 days, the patient arrives for a follow-up appointment, if necessary, a second procedure is prescribed for him in 1-4 weeks.

Cryodestruction
This method involves freezing the wart with liquid nitrogen: the moist tampon is pressed against the damaged skin (while capturing the surrounding tissue a few mm) for 1-5 minutes. Some lesions require several treatments four weeks apart.
The main disadvantages of cryodestruction are its pain and delaying effect compared to other methods, for which only one procedure is often sufficient to remove them.
Electrocoagulation
Under the influence of electric current, the wart is removed in layers. Such an operation is performed under local anesthetic.
This method is more efficient than cryodestruction, but has a significant drawback: electrocoating often leaves scars behind the site where a wart is removed. For those patients who are trying to correct a cosmetic defect, no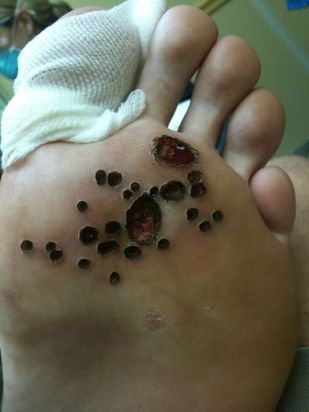 this method is the most suitable.
this method is the most suitable.
Laser deletion
The laser also removes warts in layers. The light guide makes contact with the skin from a few seconds to three minutes, depending on the size. The visible scab is then excised, and the bottom of the wound treated with laser again. The patient is then instructed how to handle the wound. The operation itself is performed under the influence of local anesthesia.
Radiowave Surgery
Radio wave surgery is one of the most modern and gentle methods for removing a number of benign neoplasms, including warts.The method is based on the generation of electromagnetic waves with different frequencies: from 100 kHz to 105 MHz. During the procedure, the tissues persist in passing waves, which is why molecular energy is released in the cells, which pass through the skin. Under the influence of heat, the cells actually evaporate - a neat cut is obtained. At the same time, no mechanical forces are applied to the affected tissue.
Advantages of this method:
- security
- ;
- fast wound healing;
- good cosmetic effect - scars and scars are excluded;
- lack of relative pain - local anesthetic is applied before minor surgery; Exclusion of secondary infection
- due to automatic disinfection of the electrode when the device is turned on.
The effectiveness of this method is recognized worldwide, however, it is relatively difficult to find a clinic that uses the method of radio wave surgery.
What treatment method to
to selectEach of the above methods has some disadvantages:
- In the first few weeks, the area worked looks unattractive - claws, dark of tissues. This should be taken into account if the warts are on visible parts of the body (for example, on the face). Unpleasant smell and a certain amount of pain during surgery.
But the main drawback isthere is a high probability of relapse, especially if the warts were widespread. With each of these methods, doctors do not fight the root cause of the disease, but its consequences, since today. cure human papillomavirus virus.
Thus, therapy focuses on:
- or deletion of neoplasms that appear at the site of introduction of the virus;
- either to stimulate antiviral immune response;
- or a combination of these types of approaches.
Destructive treatment methods are often used. Their efficiency reaches 50-80%.
Childhood is not usually a contradiction to surgical treatments. Therefore, many of them (including radio wave surgery) are used to treat warts in children. Chemical removal of warts is an exception due to the potential for adverse reactions to the substance.
What to do after the operation
After any of these operations, be sure to follow your doctor's recommendations.
After removal of the tumor by any of the methods presented, the doctor usually prescribes the treatment of the transfer site. It is forbidden to remove "crusts" by yourself, wet the wound and expose it to direct sunlight.
If a patient has persistent warts, then he should consult an immunologist - he may need drug therapy, which will increase the resistance of immunity against the manifestations of the human papillomavirus virus.
Forecast. Cosc
If the patient does not have immunodeficiencies, then the warts can go away on their own, but this will take a long time - from several months to several years. Thus, in 65% of cases, warts return independently within two years. If the wart is still in place after two years, it is recommended to remove it. It is recommended to remove multiple growth immediately.
With normal immunity and a properly selected transfer method (depending on the size and type of wart), it is possible to remove pathogenic tissue and achieve a good cosmetic effect. With reduced immunity and other predictable factors, it is caused by the remaining human papillomavirus virus in the body.
There is no specific disease prevention. But is the infection so inevitable?
Following a few rules can reduce the likelihood of a virus occurring:
- Avoid walking barefoot in public places where there is a potential for skin injury and virus infection (swimming pools, public showers, gyms).
- Choose high quality footwear, change it frequently. Try to keep your feet dry. Heat and moisture are excellent breeding grounds for human papillomavirus virus.
- To avoid periungual warts, go to a certified nail technician for manicure and make sure they use sterile tools.
To prevent anogenital warts, according to the WHO (World Health Organization), a quadruple vaccine against human papillomavirus virus is also very effective. There are currently no vaccines available to prevent other types of warts.
If you find one wart, do not try to warn yourself, cut or pick it out - this way you can contribute to inflammation and further spread of the virus along the skin. After such a "removal", instead of one wart in the morning, you can wake up ten.















































































